Recent report blames poor nutrition for diseases of civilization

Part of the message I conveyed in my last article was that our modern, westernized welfare diet is clearly out of synch with the nutritional elements our bodies require.
I am indebted to another report, “Towards a Seaweed Based Economy,” prepared by Blue Green Technologies in the Netherlands. Authors van Ginneken and de Vries outlined that, for macro-nutritional elements, the consequences of obesity and its burden of chronic degenerative welfare diseases demonstrate the required micro-elements (vitamins and minerals) for a proper mitochondrial functioning.
Mitochondrial disruption, lipid peroxidation and release of inflammatory cytokines are considered the major causative mechanism for our modern welfare diseases (mainly Type-2 diabetes and cardiovascular diseases.
In respect to mitochondrial disruption, this is very much in line with the work of New Orleans-based neurosurgeon Dr. Jack Kruse.
Nutrition and pandemic chronic diseases
To strengthen the perception that poor nutrition is the major cause for the pandemics of obesity and its burden of chronic degenerative welfare diseases, the authors listed some very familiar food products from well-known, global operating fast-food companies, highlighting the lack of vitamins and minerals in our daily eaten food, like hamburgers, fried chicken, pizzas and convenience meals.

They also discuss the nutraceutical composition of a Paleolithic diet containing all the essential vitamins and minerals for our two million years of “metabolic machinery” and quote several clinical human studies where it is demonstrated that the Paleolithic diet works. And finally, they raise the issue of integrated multi-trophic aquaculture (IMTA) with an emphasis on vitamin- and mineral-rich seaweeds.
The IMTA connection is very much in tune with the new thinking about the importance of the “circular economy.” Our current economic model – based on linear take-make-dispose – relies on large quantities of cheap, easily accessible materials and energy, and is reaching its physical limits. A circular economy is all about a continuous positive development cycle that preserves and enhances natural capital, optimizes resource yields and minimizes system risks by managing finite stocks and renewable flows.
The authors also mention that the world has experienced in the last three decades an epidemiologic transition in the leading causes of death, from infectious disease and acute illness to chronic disease and degenerative illness or from a period termed the receding famine pattern to one dominated by nutrition-related non-communicable diseases (Popkin 2003).
Clearly depicted in Fig. 1 for the macro-nutrients: total-, trans- and saturated-fat and in addition the temporal patterns of essential polyunsaturated fatty acids (PUFAs), the omega-3 and omega-6 patterns which they raised earlier, discussed and tabulated in van Ginneken and de Vries (2015). In this they focus on essential vitamins and minerals, of which the decline of the antioxidants Vitamins C and E during the course of human nutritional evolution is clearly visible (Fig. 1).
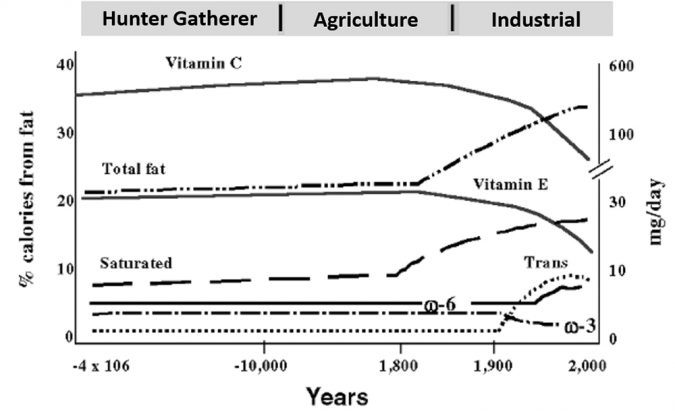
Diseases of civilization
Many so-called “diseases of civilization” have emerged, from our ancient history as hunter-gatherers and the evolving, genetically determined metabolic machinery along with the mismatch between our nutritional, cultural and activity patterns of contemporary Western populations starting around 10,000 years ago with the Agricultural Revolution.
This cluster of chronic inflammatory degenerative westernized welfare diseases, such as metabolic syndrome, obesity, insulin resistance and/or Type-2 diabetes, hyperlipidemia, hypertension, atherosclerosis, kidney failure, blindness, leg amputations and a high risk of heart attack and stroke – and recently also some mental disorders like mainly dementia and mild Alzheimers – all have the same characteristics: They are slow in progression and long in continuance and often related to this cluster of diseases (WHO/FAO 2002).
Over the past quarter-century, obesity and cardiovascular diseases have increased dramatically in the United States (Fig. 2). They are partly determined by genetic predisposition but to a major extent by environmental factors (gender, age, ethnicity), but mainly by poor nutrition, which we tabulated for macro-element nutritional food composition in van Ginneken and de Vries (2015).
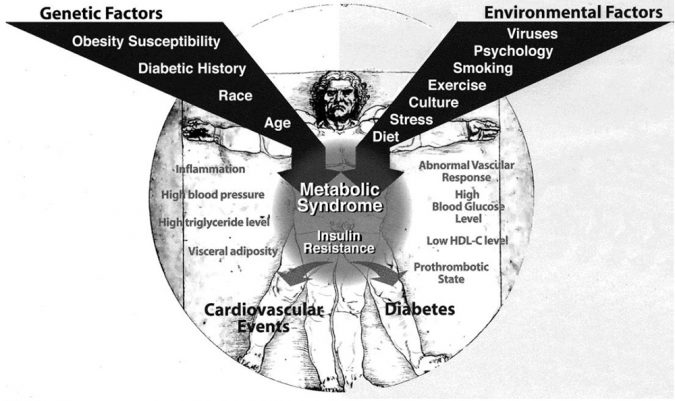
Rates of Type-2 diabetes are rising dramatically across the globe, threatening both individual health as well as the stability of national health systems according to the International Diabetes Federation. In the United States, Type-2 diabetes is the leading cause of adult blindness, kidney failure, and non-traumatic amputations (Fig. 3).
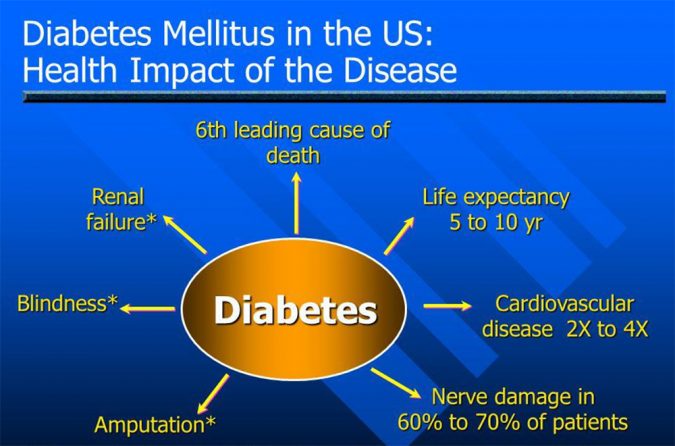
Staggeringly, estimates indicate that diabetes currently affects nearly 24 million people in the United States and that this number will rise to more than 44 million individuals by 2034. The federal debt in the United States due to Type-2 diabetes and its burden of chronic diseases, which surged past $15 trillion in 2011 (Fineberg 2012), exceeded the entire U.S. annual GDP, according to 2011 World Bank data.
While these costs are presently unsustainable in the United States – where the healthcare infrastructure is robust and relatively well-funded – the burden of Type-2 diabetes in the developing world may be catastrophic. In addition, within its burden is the development of cardiovascular diseases and stroke, the leading killers at present.
Each year, more than 2 million Americans have a heart attack or stroke, and more than 800,000 of them die. Cardiovascular diseases are the leading cause of death in the United States and the largest cause of lower life expectancy among African Americans (Frieden & Berwick 2011).
Current projections by the IDF and WHO estimated in developed and developing countries across the globe that a staggering number of individuals are currently dealing with complications of disrupted lipid homeostasis: 1.6 billion adults are overweight, 400 million are obese, and 180 million are insulin resistant or have Type-2 diabetes. The parallel growth of overweight and obese with Type-2 diabetes is striking and probably like the other diseases can be ascribed to inflammatory mechanisms with a role for reactive oxygen species.
What to do?
Based on the idea that healthy nutrition has direct impacts on medical costs, the authors give two recommendations to transform our modern, terrestrial, mono-stock agricultural system with its tremendous lack of essential macro-nutritional elements (van Ginneken and de Vries 2015), and, in addition, micro-nutritional elements. By further implementation of the IMTA food-production systems they say, hopefully, we can prevent and stop the predicted pandemic of insulin resistance and Type-2 diabetes, but also other costly chronic diseases among the obese and aging human populations.
Importantly, the authors say we must be aware that a proper solution lies in the field of a blending with a multi-focus scope knowledge from research areas like agriculture, aquaculture, medicine and new approaches like “seaweed-based practices” to generate energy from solar irradiance. Recent advances and collective and massive reformations in the mentioned research areas for the next three decades are a challenge for their organization. In many ways, this is back to the future because for thousands of years and in many cultures, seaweed has been used for food and fertilizer.
Perspectives
In closing, van Ginneken and de Vries try to convince policy makers and a wide range of professionals that, indeed, the eight millennium goals really can be reached in this century. They see this as their mission and challenge and are looking to be supported and to some extent granted by the policymakers and international organizations. We all need to get on this bandwagon and help support this activity as it is in our best interests.
References available from author.
Author
-

Roy D. Palmer, FAICD
GILLS
2312/80 Clarendon Street
Southbank VIC 3006 Australia
www.seafoodprofessionlas.org[160,194,109,111,99,46,108,105,97,109,103,64,100,121,111,114,114,101,109,108,97,112]
Tagged With
Related Posts

Intelligence
Healthy populations wanted: U.S. guidelines get it right
The 2015 "Dietary Guidelines for Americans" suggest eating at least 8 ounces of seafood per week, and advise pregnant and breastfeeding women to eat 8-12 ounces weekly. It's about time.

Intelligence
For healthy eating, we are what we allow
Many current eating habits have negative results for our health, lending credence to “you are what you eat.” Eating habits can be changed, and increasing seafood consumption can provide numerous health benefits, including as a significant source of critical micro-nutrients, vitamins and minerals. Seafood should have its own spot in our dietary food pyramid.

Intelligence
Doctors: Place a greater value on seafood consumption
Many important organizations around the world fail to acknowledge the importance of seafood to human health and well-being. There is a disconnect between what we know regarding the benefits of seafood and what is being done to acknowledge these benefits and increase seafood consumption in nutrition.

Intelligence
With seafood, health is definitely on the menu
Surveys show that fresh and healthful food, with ingredients perceived to be natural, is key for younger generations. This represents opportunity to grow seafood consumption among younger, better-informed consumers, but also a challenge to enhance sustainability.

